As a hospital, we understand the importance of emergency services and the critical role they play in providing immediate medical care to patients in need. Our emergency department is staffed by highly trained medical professionals who are dedicated to providing the best possible care to patients in critical conditions.
Our hospital is open 24 hours a day, 7 days a week to provide medical care to patients in need. Emergency departments are open around the clock to provide urgent care to patients with life-threatening conditions.
General Surgery is a field of medicine that focuses on the surgical treatment of a wide range of medical conditions. It involves performing surgical procedures on the body to treat conditions such as trauma, tumors, infections, and deformities.
Learn MoreOrthopaedics and Trauma is a medical field focused on diagnosing, treating, and preventing musculoskeletal system conditions, including bones, joints, ligaments, tendons, muscles, and nerves. These conditions may result from age, injury, or disease.
Learn MoreOur pharmacy is open 24/7 to provide you with access to medications at any time. We understand health emergencies can happen anytime, and we are here to provide you with the support you need when you need it most.
Learn MorePhysiotherapy is a healthcare profession that aims to promote movement, reduce pain, and improve body function using exercise, manual therapy, and education. Physiotherapists treat individuals of all ages and abilities with various conditions.
Learn MoreOur 30-bed facility provides 24/7 emergency and trauma care, with a dedicated team of professionals. Patient comfort and safety are our top priority. We have access to all hospital resources and strive to provide excellent care at an affordable cost to save lives and promote recovery.
Learn MoreIVF (In vitro fertilization) is a fertility treatment where eggs and sperm are combined outside the body and then transferred into the uterus. It’s usually done in a hospital setting and can help couples struggling with infertility to conceive a baby.
Learn MoreIn an emergency, every second counts. At our hospital, we know that having access to blood can be the difference between life and death for many patients. That’s why we’re proud to offer a 24/7 blood bank, always ready to provide the blood products our patients need.
Emergencies can happen at any time, day or night. Having a 24/7 blood bank means that our hospital is always prepared to respond quickly to any situation that requires blood products. This can make a huge difference in the outcome for our patients.
Our blood bank is staffed by trained professionals who are responsible for collecting, testing, and storing blood products. When a patient needs blood, a physician will place an order with the blood bank. The blood bank will then provide the appropriate product, based on the patient’s needs and the physician’s order.
Safety is our top priority when it comes to blood products. All of our blood products are carefully screened and tested to ensure they are safe for use. We follow strict protocols for the collection, storage, and distribution of blood products to minimize the risk of infection or other complications.
If you or a loved one needs blood products, your physician will place an order with the blood bank. Our staff will work quickly to provide the blood products you need and will keep your physician informed of your progress.
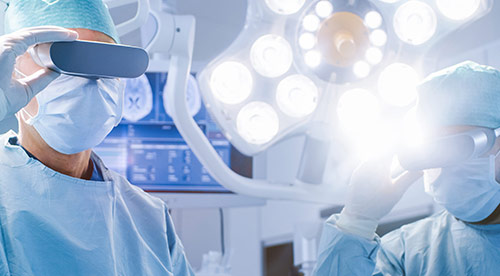
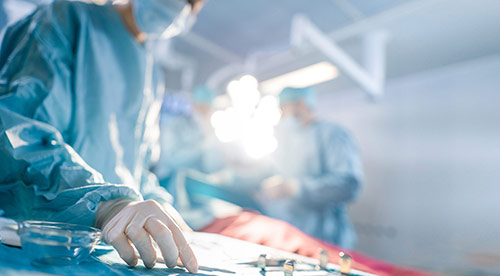
As a Managing Director and a doctor in the surgery department of this hospital, I am filled with joy and pride every day. This department is a place where we make a tangible difference in people’s lives, alleviating their pain and helping them heal. It’s incredibly rewarding to work alongside such a skilled and dedicated team of surgeons, nurses, and other healthcare professionals who are all committed to providing the best possible care for our patients.
Stay up to date with the latest news and updates from our hospital by subscribing to our newsletter. Our newsletter is a great way to stay informed about important health topics, upcoming events, and new services available at our hospital.

Advanced monitoring for exceptional patient care. Trust us.

Advanced Operating Room: State-of-the-art surgical care with cutting-edge technology and highly trained staff. Your safety and comfort come first

Highly skilled and experienced medical professionals providing personalized and exceptional care.